1 The Vagus Nerve: Your Body’s Neural Highway
The human body contains a remarkable communication system that extends far beyond our conscious awareness. While most of us are familiar with the voluntary nervous system that allows us to move and interact with our world, beneath this conscious layer lies an equally important but often overlooked network: the autonomic nervous system. At the heart of this system is the vagus nerve—a complex neural pathway that serves as the primary communication channel between your brain and your vital organs.
1.1 The Tenth Cranial Nerve: An Anatomical Marvel
The vagus nerve, also known as the tenth cranial nerve (CN X), is the longest and most complex of the cranial nerves. The name “vagus” comes from the Latin word for “wandering,” an apt description for a nerve that travels from the brainstem through the neck and thorax, ultimately branching throughout the abdomen. Unlike most nerves that serve a specific area, the vagus nerve’s extensive reach allows it to influence multiple body systems simultaneously.
Anatomically, the vagus nerve originates in the medulla oblongata, a region of the brainstem that controls many of our automatic functions. From there, it extends downward through the jugular foramen of the skull, traveling alongside the carotid artery through the neck. As it continues its journey, the vagus nerve branches extensively, sending fibers to the pharynx, larynx, trachea, heart, lungs, stomach, intestines, and several other organs.
This extensive network makes the vagus nerve unique in its ability to transmit information bidirectionally—both from brain to body and from body to brain. Approximately 80% of vagal fibers are afferent (sensory), carrying information from the organs to the brain, while the remaining 20% are efferent (motor), sending signals from the brain to the organs. This predominantly sensory nature of the vagus nerve underscores its critical role in providing the brain with moment-to-moment updates about our internal state.
1.2 The Parasympathetic Commander: Regulatory Functions
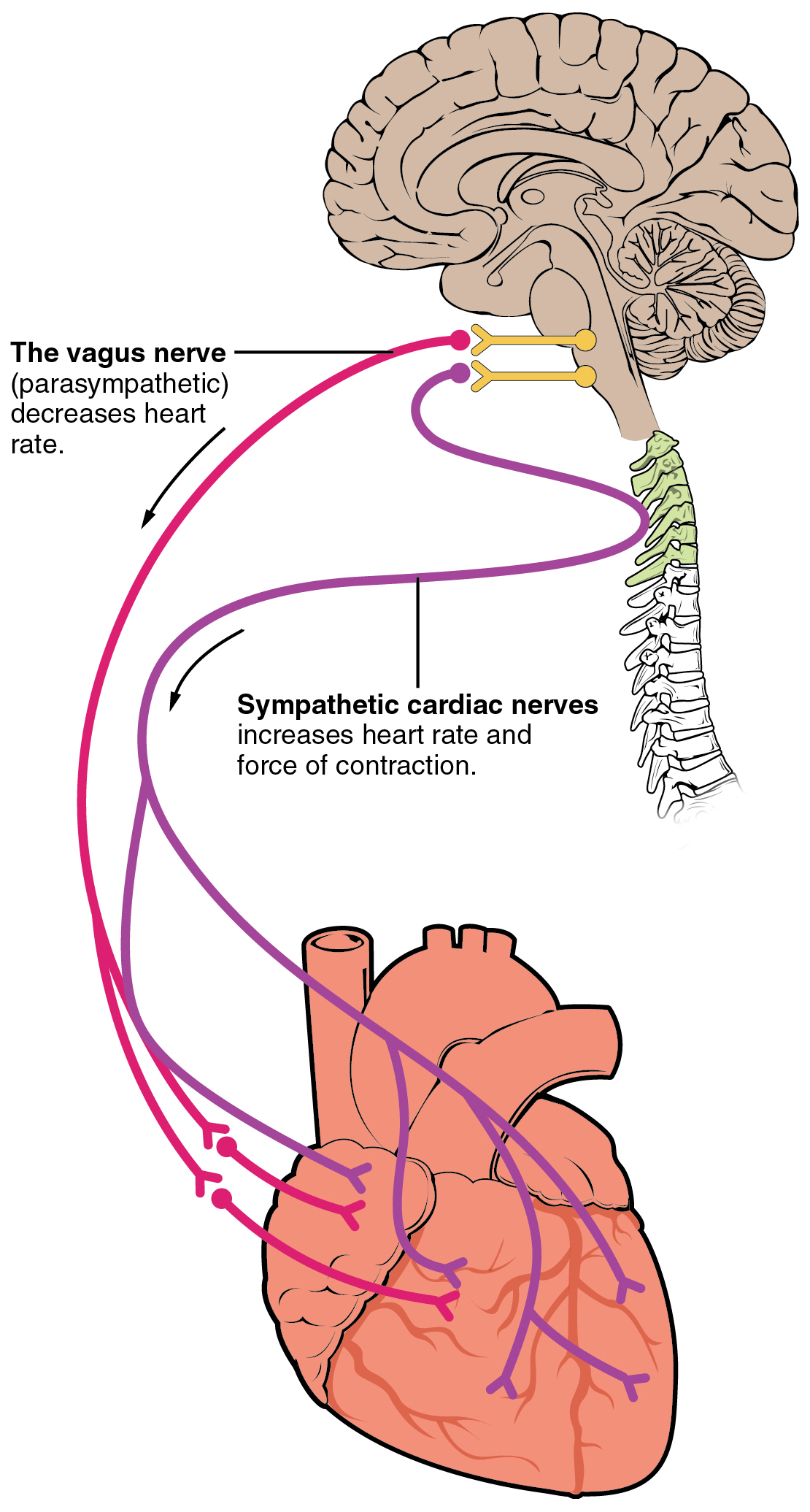
The vagus nerve serves as the primary component of the parasympathetic branch of the autonomic nervous system—often described as the “rest and digest” system. In contrast to the sympathetic “fight or flight” system that prepares the body for action in the face of stress or danger, the parasympathetic system promotes states of calm, relaxation, and recovery.
Through its efferent pathways, the vagus nerve helps regulate numerous vital functions:
Cardiovascular Regulation: Vagal stimulation typically slows heart rate and can reduce blood pressure. This “vagal brake” on the heart is essential for cardiac efficiency, allowing the heart to rest between periods of exertion. Greater vagal control of the heart is associated with better cardiovascular health and resilience.
Respiratory Control: The vagus nerve innervates the muscles of the pharynx, larynx, and bronchi, influencing breathing patterns and vocal activity. It helps modulate respiratory rate and plays a role in the cough reflex, protecting the airway from foreign substances.
Digestive Orchestration: Perhaps most extensive is the vagus nerve’s influence on the digestive system. It stimulates the production of gastric acid and digestive enzymes, increases gut motility, and controls the movement of food through the digestive tract. The vagus nerve is essential for proper digestion and nutrient absorption.
Immune Modulation: Research has revealed that the vagus nerve plays a crucial role in what’s known as the “inflammatory reflex.” Through this pathway, the vagus nerve can detect inflammatory molecules in the body and trigger anti-inflammatory responses, helping to prevent excessive inflammation.
Hormone Release: The vagus nerve influences the release of various digestive hormones, including insulin, which regulates blood glucose levels. It also affects the production of ghrelin and leptin, hormones that regulate hunger and satiety.
1.3 The Brain-Body Information Highway: Afferent Signaling
While the regulatory functions of the vagus nerve are impressive, equally important is its role as an information conduit from the body to the brain. Through its vast network of sensory fibers, the vagus nerve continuously monitors the internal environment, providing the brain with critical information about organ function, energy availability, potential threats, and overall physiological state.
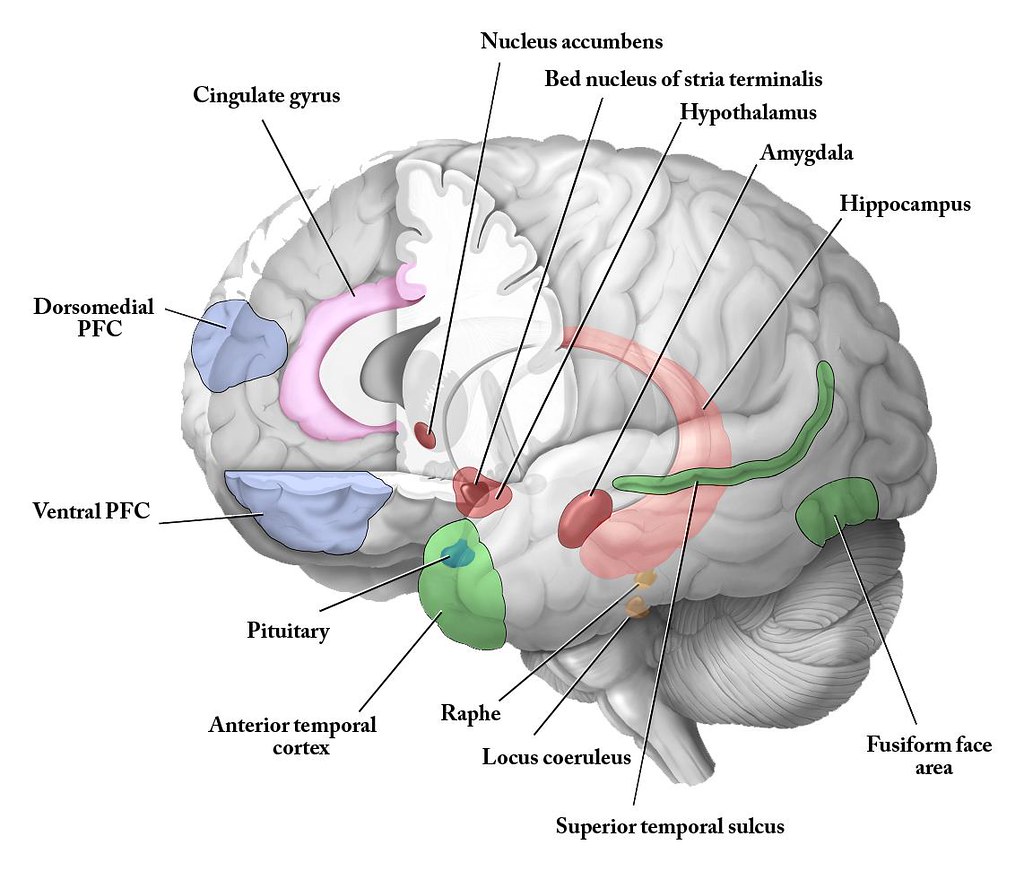
This afferent (sensory) information first arrives at the nucleus tractus solitarius (NTS) in the medulla oblongata. The NTS serves as a primary integration center, processing vagal inputs and relaying this information to various brain regions, including:
The Locus Coeruleus: A key source of norepinephrine in the brain, influencing alertness, attention, and stress responses.
The Hypothalamus: The brain’s homeostatic center that regulates hormones, body temperature, hunger, thirst, and circadian rhythms.
The Amygdala: Important for emotional processing, particularly fear and anxiety responses.
The Prefrontal Cortex: Involved in executive functions, decision-making, and emotional regulation.
Through these connections, vagal afferent signals influence not only basic physiological processes but also mood, cognition, and stress responsiveness. This explains why the state of our visceral organs—our “gut feelings”—can profoundly affect our emotional states and thought processes.
1.4 The Vagal Tone: A Measure of Nervous System Balance
The strength of vagal influence on the heart, known as “vagal tone,” has emerged as an important metric of autonomic nervous system function. Higher vagal tone is associated with greater heart rate variability (HRV)—the natural variation in time between successive heartbeats. A healthy heart doesn’t beat with metronome-like regularity but instead shows subtle variations that reflect the body’s ability to adapt to changing demands.
High vagal tone typically indicates a well-regulated autonomic nervous system that can efficiently respond to environmental changes. Individuals with higher vagal tone tend to demonstrate:
- Greater emotional stability and stress resilience
- More effective recovery from stressful events
- Better attention and cognitive performance
- Enhanced social engagement capabilities
- Improved immune function
Conversely, low vagal tone has been associated with various health challenges, including cardiovascular disease, inflammation, anxiety disorders, depression, and gastrointestinal problems. The centrality of vagal function to so many aspects of health explains why techniques that stimulate or strengthen the vagus nerve have gained significant attention in both medical and wellness contexts.
1.5 The Polyvagal Perspective: A Theory of Emotional Safety
Building on our understanding of the vagus nerve, Dr. Stephen Porges introduced the Polyvagal Theory, which provides a nuanced view of the vagus nerve’s evolutionary significance. According to this theory, the vagus nerve has two distinct branches:
The Ventral Vagal Complex: The newer, myelinated branch that supports social engagement, connection, and safety. When active, it promotes a calm physiological state conducive to positive social interactions, creativity, and health.
The Dorsal Vagal Complex: The phylogenetically older, unmyelinated branch that can trigger immobilization or “freeze” responses in the face of life-threatening danger. When dominant, it can lead to states of shutdown, dissociation, or depression.
The Polyvagal Theory suggests that our nervous system continuously evaluates risk in the environment (a process Porges calls “neuroception”), shifting between these different vagal states based on perceived safety or threat. This theory has profound implications for understanding human behavior, trauma responses, and social dynamics.
1.6 Clinical Significance: When Vagal Function Is Compromised
Disruptions in vagal function can manifest in various health conditions. Vagal neuropathy, for instance, can lead to symptoms such as persistent cough, hoarseness, difficulty swallowing, abnormal heart rate, or digestive disturbances. More subtly, reduced vagal influence has been observed in numerous chronic conditions, including:
- Inflammatory bowel diseases
- Diabetes and metabolic disorders
- Anxiety and mood disorders
- Autoimmune conditions
- Chronic pain syndromes
Recognizing the vagus nerve’s central role in health has inspired various interventions aimed at optimizing or restoring vagal function. These range from traditional practices like deep breathing, meditation, and cold exposure to modern medical approaches like vagus nerve stimulation (VNS) therapy, which we will explore in depth throughout this book.
1.7 Conclusion: The Vagus Nerve as Wellness Barometer
The vagus nerve stands as a remarkable example of the brain-body connection, serving as both regulator and informant in the complex dance of physiological function. Its extensive influence—touching nearly every major organ system—makes it a critical factor in our overall health and well-being.
As research continues to uncover the vagus nerve’s many roles and relationships, it becomes increasingly clear that vagal function serves as a kind of barometer for our physiological and psychological wellness. By understanding and supporting healthy vagal function, we open new possibilities for addressing a wide range of health challenges and optimizing human performance.
In the chapters that follow, we will explore how modern science is harnessing the power of the vagus nerve through various forms of stimulation, offering promising approaches for everything from stress management and cognitive enhancement to sleep improvement and emotional regulation.